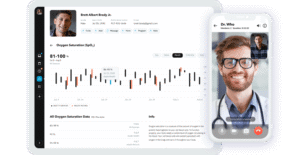
Unfortunately, the digital healthcare experience hasn’t been very good to date, especially in the US. This is due to different pieces of information being spread across multiple organizations and ecosystems. Consequently, healthcare is hard to navigate, and it’s difficult for healthcare providers to engage patients and retrieve information.
The Center for Connected Medicine (CCM) interviewed 70 leaders at 65 US health systems for their Top of Mind report. It revealed that fewer than one in three interviewees believe their organization is providing a best-in-class digital experience for patients.
Consumers are used to the experience they get with services like Amazon and expect the same convenience from healthcare providers.
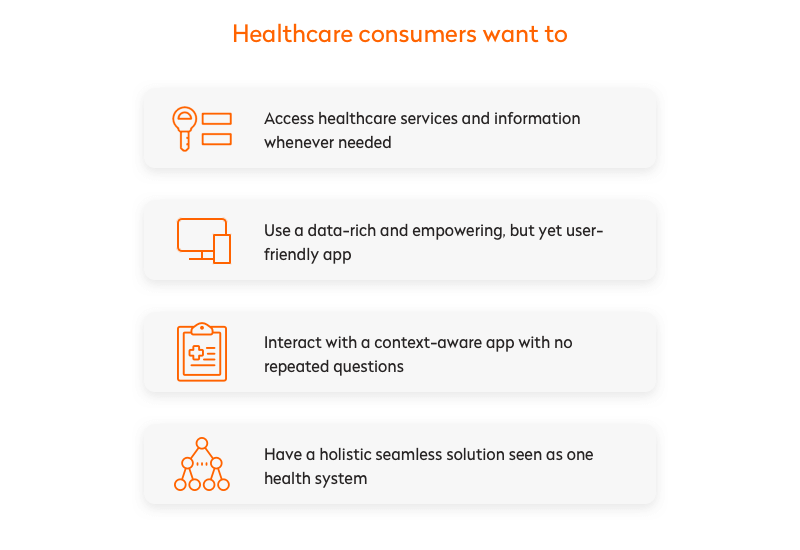
Healthcare providers have no choice but to satisfy these demands, as the industry is competitive. Providers are also looking to identify new revenue streams at additional digital access points. But the issue of interoperability among healthcare systems drastically restrains these ambitions.
How does a lack of healthcare interoperability impact the consumer experience?
Do you feel successful at sharing data within your health system? What about sharing medical information with payers, patients, and other health systems and partners? If you answered no to one or both of these questions, we aren’t surprised.
In a survey by CCM, almost one-third of hospitals and health systems reported their interoperability efforts were insufficient, even within their own organizations. Moreover, this research found that providers feel most successful at sharing data within their own health systems and less often report success sharing medical data with other systems.
These results suggest traditional healthcare providers could lose ground to more tech-savvy competitors. So how can you catch up? Building a healthcare app with the help of an API is likely to solve most interoperability and patient service issues.
You might use an existing open healthcare API to create a wide range of healthcare apps like those that help patients manage chronic diseases, allow patients to schedule doctor appointments, and even help with new clinical trials.
You might also choose custom API development to meet your healthcare system’s specific needs.
What are the benefits of APIs in healthcare?
Medical APIs (Application Programming Interfaces) help information systems communicate and transfer data between each other.

Medical app development supported by additional healthcare APIs provides the following benefits:
For developers
Developers can use predesigned API integration tools and features that facilitate app development. This saves the project budget and speeds up the time to market. For example, AdvancedMD has more than 40 templates for multiple specialties and workflow optimization. Developers can customize them and add all the functionality they need.
For hospitals
APIs help healthcare providers improve the usability of electronic health records with the assistance of third-party software for clinicians. With APIs, doctors can finally know that all patient history is consolidated in one place and is easy to access.
APIs like Eviti Web API enable doctors to decide on the most appropriate treatment based on an individual’s diagnosis and type of health insurance. APIs like DrChrono also help doctors bill patients and manage appointments.
For scientists
APIs improve international collaboration and ensure fast access to information. This facilitates medical research. If there weren’t APIs, researchers would conduct scattered studies and their results would come much slower. APIs help medical scientists quickly process the results of multiple studies, assist in discovering advanced therapies, and research the development of genetic and chronic conditions.
Platforms like GluVue are built using APIs and provide researchers with large and valuable data sets. Scientists from Stanford University have been using GluVue to remotely view continuous glucose monitoring data to improve the outcomes for pediatric patients with diabetes.
For patients
APIs allow healthcare systems to link data points from multiple systems to create more complete data sets. These data sets can then be used for quality analytics to provide better treatment results. APIs in healthcare can also allow patients to provide health records to new facilities without going through receptionists and making unnecessary phone calls.
Additionally, patients can benefit from the integration of smart devices with EHR systems, as these devices can add data to their charts and assist with diagnosis and treatment.
Thanks to the use of machine learning, services like Human API securely share real-time data with patients and healthcare providers. Human API extracts the needed data from multiple files, processes it, and analyzes it. The service is also HIPAA-compliant.
Providing top-notch security is a must when implementing healthcare integrations. Let’s pay special attention to how eHealth APIs can facilitate your software security.
How to use healthcare APIs to enhance your software security
Developers of healthcare software applications must pay close attention to ensuring security, as these apps manage sensitive personal information. Its misuse can result in disaster, from stolen identities to a patient’s death. Developers have no option but to make sure their software complies with regulations.
Most countries have their own laws protecting citizens’ health data:
- Health Insurance Portability and Accountability Act in the US
- Personal Information Protection and Electronic Documents Act in Canada
- Data Protection Act in the UK and Spain
- General Data Protection Regulation in the EU
All of these instruments regulate who has access to what’s known as protected health information, or PHI, and how this information must be managed and protected.
API security must ensure multi-level data protection and provide effective threat prevention tools. Chino.io is one platform that promises the necessary level of security for healthcare enterprises and developers offering software for US and EU healthcare providers.
Chino.io complies with current EU regulations and the data protection laws of EU Member States. Chino.io provides proprietary technology and consulting services to ensure your apps are GDPR- and HIPAA-compliant. They also provide software quality certification according to security standards ISO 9001, ISO 27001, and ISO 13485, supporting the certification of medical-grade software and devices.
In general, healthcare product engineering requires developers to take into account the following aspects of security:
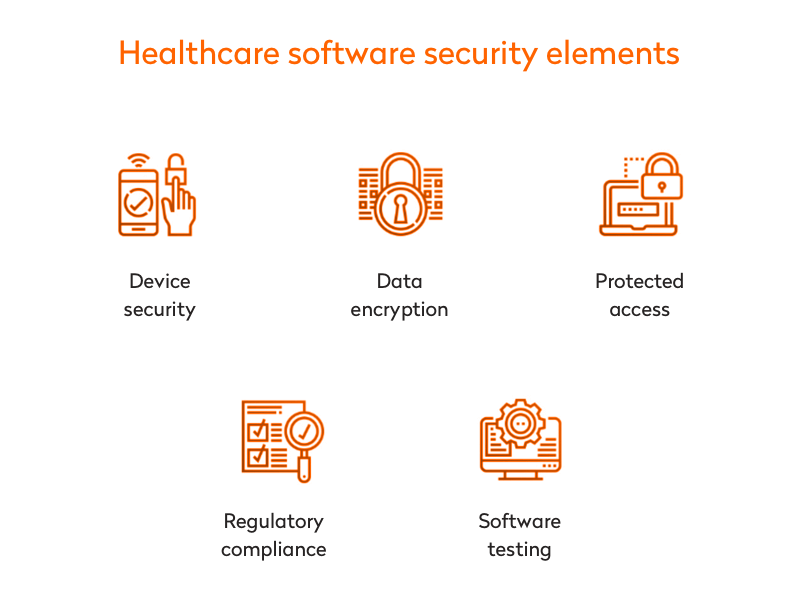
For details on software security elements presented in the image above, read our articles on HIPAA compliance and key data security technologies.
Health APIs also provide an instant connection with existing data references, such as e-records. But EHR interoperability is a significant problem faced by healthcare systems. Let’s consider.
Reasons for a lack of EHR interoperability and how APIs can address them
Despite developments in EHR technology and adoption, EHRs keep contributing to data silos that make interoperability a challenge. Hospital APIs are one of the most promising ways to address all the reasons behind the EHR interoperability mess.
Here are some of the main reasons for a lack of interoperability, data exchange, and data sharing across EHRs and other health information technology (HIT) systems:

Lack of common patient identification standards. EHRs are the key repositories and ways to access patient information. But there’s still no national patient identifier helping us recognize a specific patient within an EHR system. Issues with identifying patients and matching their records are a huge problem for healthcare providers. The result is inflated healthcare expenses, poor quality of treatment, and safety issues.
Insufficient payer participation in data sharing. There’s a terrific amount of data in the hands of payers. Having access to this data would do healthcare providers a great service, facilitating health outcomes. But payers are protecting that data industriously, as it essentially contributes to their profits, and are shifting from public to private health information exchange. This makes it harder and more expensive for providers to ensure interoperability and integration.
Lack of communication standards across EHRs. Sharing clinical information between hospitals is gaining momentum. But multi-hospital systems and networks are increasingly sharing data between different EHR systems. EHR vendors often build proprietary communication and language protocols, which block communication with other EHRs. This requires healthcare providers to somehow integrate with multiple EHRs inside and outside their own facilities.
EHR integration is costly. Lots of medical institutions are using different medical technology systems to manage protected health information (PHI). This requires them to connect and integrate with disparate EHR and HIT systems. Ensuring such a level of connectivity is so costly that only large healthcare enterprises can afford it.
Healthcare APIs have the potential to address all these problems by ensuring data and PHI sharing and communication between EHRs and HIT systems. Many of the big EHR vendors already offer open APIs to help third-party software developers build apps that access EHR data. But it’s not that simple! Due to technical, security, and regulatory barriers, integrating a third-party EHR is still a challenge.
We had to integrate a third-party EHR while developing Healthfully, one of our healthcare projects. Let’s see how we managed to overcome challenges related to this integration and ensure smooth and stable communication between our client’s system and the third-party EHR.
Yalantis’ experience integrating a third-party EHR
We had to enable the Healthfully app to exchange personally identifiable information, PHI, and information on doctor appointments with a third-party EHR system used by a partner organization. To do this, we needed to ensure smooth data transfer within HIPAA-compliant environments.
The EHR system used by our client’s partner organization is on-premises/cloud-based software that provides different communication interfaces for third-party integration partners, depending on the contract agreement. For Healthfully, two interfaces were available: an HTTP RPC-based API interface and an HL7 layer, each serving specific purposes.
Here are the main EHR integration challenges we faced and the solutions we used to properly integrate with the EHR:
Securing network communication between Healthfully and the EHR system. We established a secure VPN tunnel, connecting a hardware-driven IPSec VPN gateway on the client side with a virtual software-based VPN gateway on the Healthfully side using a software appliance (Openswan/Libreswan).
Implementing the HL7 message processing layer. We integrated with the HL7 messages interface by implementing proxy software within the Healthfully infrastructure. This software converts XML-based data into the HL7 format accepted by the EHR system and vice versa.
Implementing an RPC API processing layer. We implemented several abstraction layers on the Healthfully side. To do that, we separated the business-level architecture from specific communication data specifications used by the EHR system. This API strategy has had significant results:
- Developers can focus on the app logic rather than on dealing with the third-party data format and data flow specifics.
- Healthfully can easily onboard new partners with their own EHR systems. This allows Healthfully to focus on developing new communication adapters for every specific EHR system while retaining common business logic across organizations.
We used the same modular approach to successfully implement all third-party integrations within the Healthfully app, including payments and a telemedicine solution.
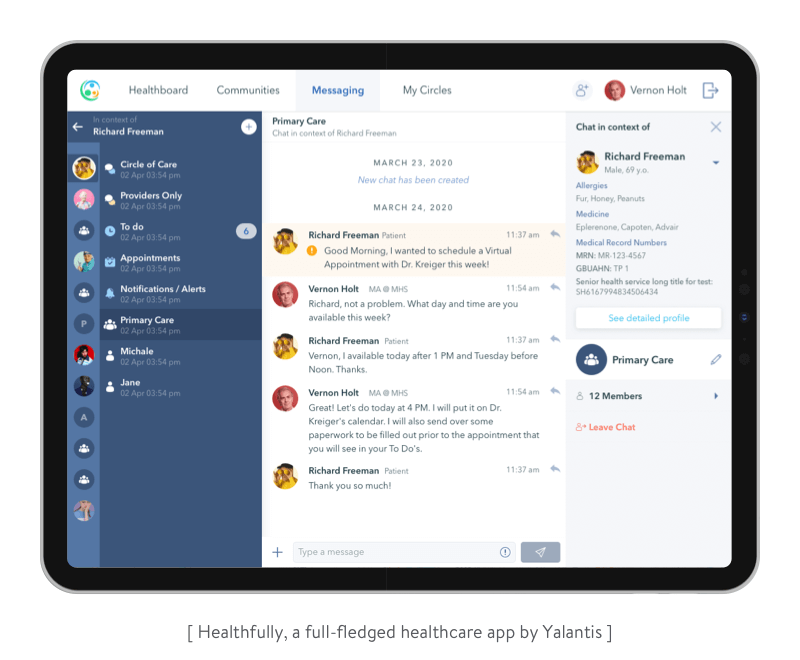
Medical APIs have helped developers with sending, retrieving, and processing data. But as you can see from our EHR integration API experience, APIs alone can’t solve all the technological issues and lack of data standards in the industry. But it seems like a light has appeared at the end of the tunnel.
What the future holds for healthcare interoperability: How APIs keep disrupting the industry
This spring was marked by an optimistic outlook for the healthcare industry and software developers when the US Department of Health and Human Services released its final rules regarding interoperability, data sharing, and patient access.
Implementation of a Patient Access API
Starting in 2021, Medicare Advantage, Medicaid, the Children’s Health Insurance Program, and plans participating in the federal exchanges will have to support a standardized API (HL7 FHIR version 4.0.1). This API will help patients access claims and their clinical data via any third-party app they choose. This API might also be used to integrate a health plan’s data into a patient’s EHR.
Adoption of a Provider Directory API by CMS-regulated payers
The adoption in 2025 of a Provider Directory API among CMS-regulated payers also promises to benefit developers and the healthcare industry as a whole. This API is tailored to help third-party app developers provide patients with a variety of healthcare providers to choose from. The Provider Directory API will enable healthcare providers to find other providers for coordinating patients’ treatment.
This unified standard will significantly simplify developers’ work as they’ll no longer have to adjust their software solutions for different CMS-regulated payers.
These US government initiatives are likely to enable app developers to provide healthcare consumers with the same top-notch experience they already have managing their finances, travel, and shopping. The most exciting part of the history of APIs and medical innovation is yet to come, but mature modern medicine software providers are already experienced and brave enough to solve any integration challenge.